Adapting to Climate Change (Part 1): Health Care
finding diagnostics solutions for vector-borne diseases
Editor’s note: The Asian Cities Climate Change Resilience Network (ACCCRN), supported by the Rockefeller Foundation and composed of 10 cities in India, Indonesia, Thailand and Vietnam, assists businesses as they seek ways cities might prepare for, withstand and recover from impacts of climate change. Intellecap is supporting these private-sector interventions and mapping pilot project results across various sectors. This blog, the first of a three-part series, looks at health care solutions. Part 2 will look at sustainable affordable housing and Part 3 at non-life microinsurance.
The impact of global warming has led to shifts in rainfall patterns and increased flooding which have resulted in an increase in the incidence of vector-borne diseases like malaria and dengue, and infections by other groups of viruses that are primarily transmitted by arthropod vectors. There were an estimated 627,000 malaria deaths worldwide in 2012. In addition, an estimated 390 million dengue infections occur per year across the globe. Although the entire global burden of dengue is uncertain, there has been a sharp rise in the number of cases reported in recent years. The World Health Organization estimates 22,000 deaths occur yearly, mostly among children. Thailand reported the worst dengue outbreak in 20 years, with 126 deaths and 135,344 people infected with the virus, in October 2013.
The population at the bottom of the pyramid is most affected by vector-borne diseases due to their living conditions, poor housing and lack of resources. Malnutrition and sleeping outside or on the ground increase the risk of becoming infected. Poverty can also increase the progression of the disease, worsening illness and leading to death, mainly through poor nutrition and weak immunity.
Lack of access to information and limited education are major barriers faced by the poor in accessing health care facilities. These, in turn, influence perceptions of health and illness, health-seeking behavior, and compliance with therapy, thus depriving the poor of quality health care. The cost of travel to access quality health care is also a limiting factor.
In India, government-sponsored programmes for prevention and control of these diseases have implemented many interventions at all levels, including the community level. However, the key challenge has been in effective and timely diagnosis of the diseases along with affordable treatments. The ideal scenario is to bring in private players by adopting a sustainable business model targeted at the poor.
Private sector: Redefining health care delivery
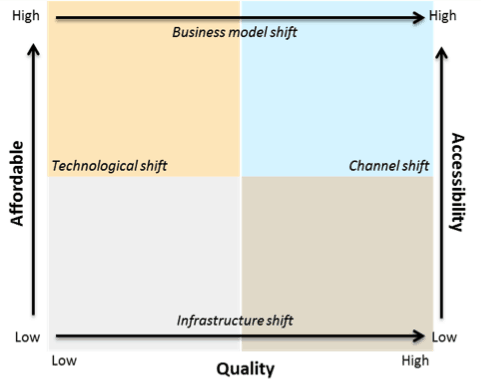
Intellecap’s health care trend model
Primary health care issues faced by most Indians at the bottom of the pyramid include accessibility, affordability and quality of health care. Intellecap has observed shifts in the way the health care industry operates in India. For example, improvement in infrastructure has led to significant improvement in the quality of health care in certain pockets of the country. Technology-driven improvements such as non-invasive technologies, software-based applications, etc., have improved the affordability of diagnostics and health care services. Similarly, business model shifts by organizations such as Aravind Eye Care and Vaatsalya have made quality health care services affordable for many in the low-income group. However, affordability, quality care and accessibility remain a colossal challenge across the country. Where there is a paucity of qualified health care personnel, corporate interventions through technological innovations, disruptive business models and channel shifts could bring about a paradigm shift in the health care industry.
Given the above context and challenges, Intellecap, along with Bosch Healthcare Ltd., aimed to establish the feasibility of using reliable and affordable diagnostics solutions for vector-borne diseases through a pilot study. Currently, diagnosis for detecting malaria is done through microscopic examinations, rapid diagnostic tests (RDTs) and polymerase chain reaction (PCR). Microscopic examinations are highly dependent on the skill set of those conducting the tests and there is also a delay in providing results. RDTs are more accurate than the regular microscopic examinations and provide immediate results. Further, RDTs have made screening affordable to the masses; each test costs less than 50 cents. But sensitivity varies depending on the manufacturer and RDTs cannot differentiate between different kinds of malaria. PCR provides accurate results but is significantly more expensive and not easily accessible.
Our research showed that reducing the price is not the only solution to solve the health care woes at the bottom of the pyramid. Some of the most inexpensive methods of diagnosing vector-borne diseases, like the RDT for malaria, are highly unreliable. Further, even if the consumer is willing to pay for a better quality product, the service providers – namely the doctors and diagnostic centres – should have the capital and the willingness to invest in new technology.
Learning from the field
The pilot study highlighted the challenges that mainstream corporate firms face when attempting to resolve health-related issues at the BoP. The majority of the challenges emerge during the design stage. These include investment commitment; risk of directing resources toward diseases with reducing prevalence (but which remain prevalent in low-income groups); ensuring financial feasibility; and the threat of substitution.
Even after developing a product or service, corporates face issues in commercializing their solution. They are often posed with challenges relating to the size of the addressable market, price point, and time lag between innovating and commercializing the products, amongst other problems.
A few of the initiatives which can help overcome these challenges are:
Market estimation. It is vital to undertake the market estimation exercise early during the innovation cycle. Corporates should identify their target population, its size, seriousness of illness, willingness to pay, alternative solutions, etc., before designing the product. These studies can also help provide inputs which can be incorporated during the design stage.
Bundling of services and technologies. During the innovation stage, corporates should identify diseases/illnesses which are similar in nature and which have similar diagnosis procedures. This, apart from providing a larger target market, also ensures optimization of costs related to development and transportation, thus improving viability.
Develop channel partners. Private players should involve experts/consultants who understand the requirements of the target population. The experts can also leverage their existing network and channel partners during the pilot and launching of the products.
The study revealed that technological innovations alone cannot resolve health care-related issues at the bottom of the pyramid. Before developing a health care product for the BoP, private players should look into many aspects, like the challenges in commercialization and workarounds required, partnerships with nontraditional partners, solutions for multiple uses, and user friendliness, as the users may be relatively unskilled. These strategies can help ensure the sustainability of a low-cost business model serving the poor.
Photo: With the world’s second-longest national coastline, Indonesia is highly vulnerable to flood. Photo courtesy of ACCCRN.
Nisha Dutt is the CEO at Intellecap and also leads Consulting Services.
- Categories
- Health Care
