A ‘Win-Win-Win’ Possible In TB Battle: But engagement with private providers is critical for achievement of goals
As associate director of the McGill International TB Centre in Montreal, Dr. Madhukar Pai’s research is mainly focused on improving the diagnosis of tuberculosis, especially in high-burden countries like India and South Africa. He recently answered some questions, via email, from NextBillion Health Care about a few of the overarching market issues that impact efforts to diagnose and treat TB worldwide. (To watch a recent presentation by Dr. Pai at the University of Michigan, click here and check out his Q&A interview with WDI’s Prashant Yadav below.)
Kyle Poplin: How would you assess the battle to control and eradicate TB in India and around the globe today compared to, say, 10 years ago?
Madhukar Pai: Progress has been made, but the burden of TB globally, and in India, continues to be unacceptably high. There are an estimated 8.7 million new TB cases each year and an estimated 1.4 million deaths. India alone accounts for nearly 2.2 million of the new TB cases that occur each year.
Although the DOTS strategy (the World Health Organization’s recommended TB control strategy) has been widely implemented, the most worrisome issue is that the incidence of TB is declining much more slowly than expected. It is now clear that TB cannot be eliminated by 2050 (with “elimination” defined as the reduction of annual incidence to less than one case per million population by 2050).
Another big concern is reports of severe forms of drug resistance in many countries, including extensively drug-resistant TB (XDR-TB) and the so-called “totally drug-resistant” TB.
KP: What innovations in diagnosis/diagnostic tools are in the pipeline that you think will have a high public health impact?

MP: Antiquated tools have historically posed a big challenge for TB control. For example, many low-income countries still rely on the century-old sputum microscopy technique which has limited sensitivity. Thankfully, things are changing rapidly. For the first time, a rapid, cartridge-based, automated molecular test – the Xpert MTB/RIF test – is being scaled up for diagnosis of tuberculosis and detection of drug resistance to rifampicin in many countries. Nearly 3.2 million Xpert MTB/RIF cartridges have been procured worldwide in the public sector in 88 of the 145 countries eligible for concessional pricing of $9.98 per cartridge.
This month, the largest ever rollout of Xpert MTB/RIF got under way, aiming to save 62,000 lives and prevent the spread of drug-resistant strains of TB. The TBXpert project, funded by UNITAID and coordinated by WHO and the Stop TB Partnership, is worth U.S. $25.9 million and will see the deployment of more than 220 Xpert machines and 1.4 million test cartridges in 21 countries.
While modeling studies suggest that Xpert will have a public health impact, it is clear that most countries are deploying Xpert at the district level or in centralized laboratories, or reserving the test for only those with suspected drug resistance. So, it is unclear whether Xpert will actually help interrupt transmission by detecting TB early.
The Xpert technology was not designed for peripheral clinics and microscopy centers where most people with suspected TB are seen initially. So, the focus is now on developing accurate molecular tests that can be used at these lower level health centers and clinics, where they could be used in point-of-care testing programs with the goal of rapid TB treatment initiation in the same visit. Indeed, some new molecular assays have been developed for this purpose, but evidence is lacking on their field worthiness and accuracy/impact. The Bill & Melinda Gates Foundation recently made a big investment in this space. Hopefully, all this will mean a gradual transition to molecular diagnosis of TB in high-burden countries.
KP: What innovative delivery methods (i.e. ways of improving the market for these new products, innovative ways of incentivizing different health care providers) are coming? Why is it so important to involve the private sector in the battle against TB?
MP: The strategy for increasing affordability of WHO-endorsed products, thus far, has been to negotiate special prices (volume based) for the public sector in high TB burden countries. With Xpert, several donors pooled resources to buy down the price to $9.98 per test. But all of these models have consistently ignored the private sector in poor countries.
In many high-burden countries, the private sector is a major provider of health care. In India, Bangladesh, Cambodia and Pakistan, for example, 70-80 percent of first-contact care happens in the private sector. On the one hand, the private health sector is often seen as part of the problem – diagnostic and treatment practices are known to be suboptimal. On the other hand, given their dominant role in TB care, engagement with private providers is critical for achievement of TB control targets. In particular, since private providers are often the first point of contact, their involvement is critical for early and accurate diagnosis.
Thus, a key challenge in TB control is significant engagement with the private sector -– for example, replacing suboptimal tests with WHO-endorsed, validated tools at affordable prices, and ensuring that all TB cases are appropriately managed. This will require innovative business models and delivery approaches, and such models are being piloted in countries like India, Pakistan, Bangladesh and Indonesia.
In India, the Initiative for Promoting Affordable, Quality TB tests (IPAQT) has made WHO-endorsed TB tests more affordable in the private sector. In parallel, a Public Private Interface Agency pilot intervention has been launched in two cities to engage private and informal providers and incentivize them to diagnose, notify and manage TB correctly. In Bangladesh, Indonesia and Pakistan, a package of interventions, including TB care, is being offered using a social enterprise model. Hopefully, these novel approaches will work and can be scaled up.
KP: Why is the private sector particularly important in India, and can you tell us more about the IPAQT initiative?
MP: More than 80 percent of India’s health care is delivered through the private sector. Most poor people who develop a cough first seek care in the informal private sector (chemists and unqualified practitioners) rather than from qualified practitioners. Ultimately, about 50 percent of them end up in the public sector where they receive free treatment. This pathway to curative care can take from weeks to months, during which they continue to transmit infection to others. This delay, coupled with the high cost of care in the private sector, can drive families into debt. And yet, for all the money spent, patients frequently undergo inaccurate tests and inappropriate treatment. This broken pathway is a major driver of drug-resistant TB.
So, without engaging the private sector, I cannot see how India can control TB. Promptly getting patients the right test in the private sector is a critical first step for interrupting transmission. And getting private sector patients on the correct TB drug regimen with adequate supervision is fundamental for preventing the emergence of drug resistance.
In 2012, the Indian government took a bold step of banning inaccurate blood tests that were popular in the private market. This ban made it obvious that quality-assured, WHO-endorsed TB tests needed to be much more affordable if they were to replace the inaccurate, banned tests.
The Clinton Health Access Initiative stepped in and organized a group of device manufacturers and service laboratories into a partnership called IPAQT. The lab service providers agreed that in exchange for not exceeding negotiated, ceiling prices to patients, notifying the government of the cases diagnosed, promoting the use of quality tests and participating in external quality assurance, they would get reagents at significantly reduced prices. In exchange for offering lower prices, the manufacturers and distributors would receive greater and more predictable volumes from the previously untapped private market. In sum, IPAQT aspires to a “win-win-win” situation where laboratories, suppliers and patients all benefit from a shift from premium pricing to a mass-market (high-volume, low-margin) model.
I am pleased that IPAQT now has 50 private labs offering several WHO-endorsed TB tests (Xpert MTB/RIF, MGIT and BacT/Alert liquid cultures, and Hain line probe assay) at prices that are nearly 50 percent lower than the market price. These tests are now in the same price range as the banned antibody tests.
I am hopeful that more than 100 labs will be engaged by next year. But there are challenges. The market still has suboptimal tests that offer greater margins to the laboratories and health care providers, and this means they are less likely to promote WHO-endorsed tests which offer lower margins. Also, even with IPAQT pricing, WHO-endorsed TB tests are still beyond the reach of patients at the bottom of the pyramid. For the BoP, the public sector is a good, viable option since the Indian Revised National TB Control Programme has done well to reach scale and TB diagnostic and treatment services are completely free and accessible.
KP: Is India’s government investing more money in the effort to control TB? If TB is to be eradicated, what other governments or organizations must join this battle?
MP: TB control in India is a very cost-effective program. But, historically, it has been chronically underfunded. For 2012-13, for example, the Indian TB control program was allocated Rs. 710.15 crores (about U.S. $142 million), which is only 2 percent of the total health sector budget.
The Indian government recently approved the National Strategic Plan for 2012–17, which sets an ambitious goal of universal access to quality TB diagnosis and treatment for all patients in India. This goal of universal access will mean increasing the capacity to manage and treat all forms of TB, including drug-resistant TB. Meeting this goal will require substantially greater resources than what is currently allocated to the TB control program.
There is a clear disconnect between the goals and the resources required to meet the stated goals. With the steady slowdown of the Indian economy over the past few years and the current crisis with the rupee, things do not look promising in the short term. In these tough circumstances, it would be wonderful if Indian philanthropists and corporate groups stepped in and did their bit for TB control. India has many high net worth individuals and celebrities. Sadly, none have championed TB control. I keep hoping this will change.
KP: The U.S. Food and Drug Administration last year approved a drug called Bedaquiline, making it the first new TB drug approved in more than 40 years. Why are new drugs so slow to arrive on the scene? Are more coming?
MP: Yes, everyone is excited about this first new TB drug approved in more than 40 years. Other new TB drugs or combinations are expected within the next two-three years, including a moxifloxacin-containing regimen and a novel drug combination treatment (called PaMZ) containing PA-824, moxifloxacin and pyrazinamide. Shortening TB treatment to two or even four months should greatly increase cure rates, improve patient adherence and reduce the likelihood of drug resistance.
There are many reasons for the slow progress – insufficient industry interest and investment in TB, inadequate donor support, challenges in doing large-scale, expensive drug trials, a complex regulatory environment for entry of new drugs into markets, and the need to evaluate new TB drugs as combinations (regimens) rather than single agents. This is why the Critical Path to TB Drug Regimens initiative was launched. The purpose is to deliver a safer, more efficacious and faster?acting TB regimen by developing and promoting innovative regulatory science essential for supporting new combination drug development.
KP: What is most overlooked in the TB space? What are we not thinking about that we should be considering to move this field forward?
MP: In all areas of health, there is now increasing emphasis on translation. Translating basic science to get products into clinics; translational epidemiology to get policies implemented at the population level; and translational global health which can bridge the science-to-service continuum.
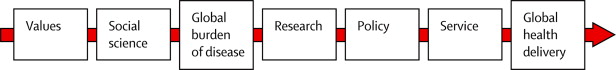
Source: Maruthappu M et al. Translational global health: from shortage to science to service. Lancet Global Health 2013
I believe the TB space needs more translational experts (“honest brokers”) who can serve to connect various segments of the pipeline and advocate for greater collaboration and cooperation, so that existing products, knowledge and policies can actually translate into saved lives and, ultimately, TB elimination.
Editor’s note: The views expressed in this interview are those of Dr. Madhukar Pai and do not necessarily represent the views of any institution with which he is affiliated.
Lisa Smith, research associate at the William Davidson Institute at the University of Michigan, recently discussed the changing face of tuberculosis and the need for treatments to keep pace.
- Categories
- Health Care
