Learning From Failure: Lessons From Nigeria About Integrating Technology Into Rural Health Systems
As part of the Millennium Development Goals (MDG) era, the Nigeria Federal Capital Territory (FCT) Administration through its Health and Human Services Secretariat and the MDG Project Support Unit sought to understand how best to improve access to health care for the majority of the people living in the territory, so we conducted a survey of accessibility to primary health care services. The survey, administered in 2008, marked an important turning point for the FCT and its nearly 3.5 million inhabitants.
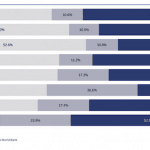
One thing quickly became clear: Business as usual would not be sufficient. The survey revealed that only 26 percent of communities had access to primary health care facilities and only 17 percent of those facilities were functional. In fact, only 179 primary health centers (PHCs) existed, and many of them were operating at suboptimal levels or located long distances from rural populations.
Closing this gap would require dramatic change in several areas, including improving infrastructure, purchasing new equipment, and building a strong and diverse health care workforce. Regional officials estimated that adequately serving the population would require constructing 434 new PHCs – nearly 2.5 times the amount that currently existed.
Such a large expansion was clearly cost prohibitive and nearly impossible, considering the limited resources. We knew we would need to take a radical approach and experiment with how technology (ICT) could help increase access to affordable, high-quality and sustainable health services.
Our eHealth journey in FCT from 2008 to the present was not always smooth, but it can certainly shed light on important lessons in integrating ICT into health systems, especially in limited-resource settings.
Mailafiya: Bringing ICT to rural primary care
The shocking survey results led to the creation of an eHealth program in the FCT called “Mailafiya,” which means “he who brings life” in Hausa. Mailafiya would integrate an eHealth component into existing primary care delivery systems, with a special focus on using new ICT tools to serve and track health data around rural, poor communities.
Mailafiya consisted of 24 field teams made up of a medical officer, a nurse midwife, a lab scientist, a driver and a community health extension worker. Each team had notebook computers provided by the Intel Corporation (a program partner) so they could capture and upload data onto a central eHealth portal that would enable health managers to visualize live health statistics from the field and undertake evidence-based interventions accordingly. Unlike typical primary care providers, each team had a customized van which served as a mobile laboratory unit with essential drugs and routine vaccines.
The initial rollout of Mailafiya saw a 270 percent increase in patients seen and a 900 percent increase in diseases reported, compared to static primary care facilities. Based on these results, the program was scaled to cover 336 communities across the six area councils and later to 13 primary health care clinics, two private secondary hospitals and three public general hospitals.
Despite its promising start, however, the expansion of the Mailafiya eHealth pilot to secondary health facilities was overcome by various challenges that eventually led to its failure. Key reasons for the failed pilot included a lack of acceptance and ownership of the project – and hence resistance to change – by health workers, low basic computer literacy among health workers, lack of sustainable funding, weak governance and regulation, and a poor state of ICT infrastructure including internet connectivity and regular power supply.
Learning from failure
The failure of the Mailafiya eHealth pilot was unfortunate, but created a unique opportunity for learning and future improvement. Lessons learned from the failed Mailafiya pilot have led to a stronger and more sustainable eHealth framework in Nigeria that will better serve millions of people for years to come and, we hope, influence how other health systems around the world integrate ICT into their health policies. A few key lessons that emerged include:
- Try and fail quickly. By implementing the pilot and scaling to select other communities relatively rapidly, we were able to more efficiently learn from our experience to adapt and improve our approach. Most of all, we were able to share learnings with others sooner rather than later; the FCT eHealth program became a case study for eHealth implementation among the 36 states of the Nigerian federation, and these lessons are contributing to a stronger understanding of how eHealth can strengthen health systems in settings with limited resources.
- eHealth tools must operate within an ecosystem. We quickly understood that as health officials we must carefully examine and align several critical pieces that need to be in place for a successful project. Often we refer to this step as building the “enabling environment” for eHealth to take place. In 2012, we reviewed the Mailafiya pilot alongside the WHO and ITU eHealth strategy toolkit and found that some of the required enabling environment components recommended in the toolkit were missing in FCT, which made it much more challenging for the program to succeed.
- Strategy, policy and standards are important prerequisites for successful eHealth rollouts. These pieces often outline a roadmap for short- and long-term success and sustainability of eHealth programs, and enable them to be more integrated within existing services and priorities.
Thanks to both reflection and collaboration, we were able to make significant progress following the failed pilot. To ensure we were taking a comprehensive approach that accounts for the entire ecosystem, for example, we convened the first FCT eHealth stakeholders meeting with various players in health and ICT, which recommended the setup of an eHealth committee and an eHealth desk in the Department of Health Planning, Research, and Statistics, in addition to an FCT eHealth technical committee. In 2013, this committee pioneered the collaborative development of the FCT eHealth policy and 2013-2015 implementation strategy document – a first of its kind in Nigeria – in our attempt to bridge the enabling environment gap for eHealth in FCT.
Looking forward: building the ecosystem
We expect that systematic adoption of eHealth in FCT in the near future will lead to universal access to high-quality, affordable, equitable and sustainable health care services. Tools including telemedicine, e-learning platforms, e-information channels and more have the power to bridge the existing gaps to basic health services between rural and urban areas – they just need to be used in the right way.
So, now, our work continues. In 2016, the eHealth committee contributed to the collaborative drafting of Nigeria’s National eHealth Strategic Framework 2015-2020, which was approved at the National Council of Health meeting. We continue to build the foundation needed beneath any health systems – including several electronic medical records projects currently at various levels of implementation – with the ultimate goal of achieving a central, integrated collaborative platform capable of harnessing data for evidence-based decision-making and health planning in the FCT through a Health Information Exchange.
We will continue lead and coordinate eHealth activities in FCT. It is our hope that with improvements, optimization, standardization and integration of existing eHealth platforms across both public and private sectors, we can, together, accelerate socioeconomic development within the FCT and serve as a role model to other health “ecosystems” around the world.
Dr. Iniobong Ekong is a desk officer of eHealth at the FCT Health and Human Services Secretariat in Nigeria. The author would like to thank Emeka Chukwu for his role in contributing to this article.
Photo of Mariam and Uche, a statistician and a software developer in Lagos, by the UK Department for International Development via Flickr.
- Categories
- Health Care, Technology
- Tags
- data, failure, rural development