Sterilization Trumps Disposable: Pre-packaged instruments place ‘huge burden’ on remote facilities
Editor’s note: This is part of a series on NextBillion Health Care regarding the lack of safe, basic surgery in much of the developing world. The first installment can be found here.
Imagine if every time you went to a hospital for care, you faced a high risk of a life-threatening infection. Imagine if even the most fundamental methods of infection control were unavailable, making routine and essential procedures, such as a cesarean section, extremely risky. How would you balance the risk and how would you feel if you knew that procedures that others in the world take for granted as safe and effective posed such a threat?
In the U.S., or any other high-income nation, surgery is never performed without sterilized instruments. The elimination of all microorganisms before an object comes into contact with human tissue was a turning point that allowed surgery to shed its dangerous reputation and enter the modern era. As a result of the introduction of anesthesia and sterilization, lives are routinely saved and disabilities are averted by straight-forward surgical procedures that pose minimal risk. Today in the developed world, we take for granted that a mother will not succumb to obstructed labor, a wounded limb will not result in permanent disability, and a hernia will not prevent a man from working for the rest of his life. Conditions like obstetric fistula have become obsolete in the developed world because they can be reliably prevented by simple surgery provided at the primary care level.
Yet the reality is very different in many parts of the world, where simple surgical care can be a risky undertaking. In low- and middle-income countries (LMICs), 16.5 million people die every year because they don’t have access to this care. And the conditions these people are unnecessarily dying from – largely non-communicable diseases, injuries and childbirth complications – are on the rise.

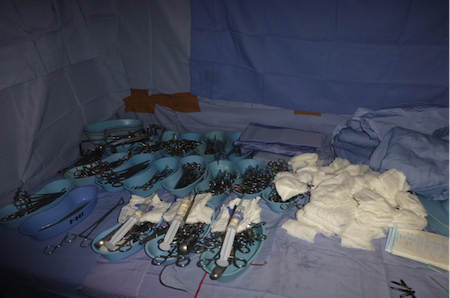
(Chemical disinfection during a free health care outreach by Pro-Health International, left and below.)
Despite the large burden, less than 4 percent of the world’s surgical procedures are performed in low-resource countries, where the basic requirements for surgical care – standards such as use of sterile instruments – are impossible to achieve in a primary care setting. As a result, surgical care that should be simple and safe carries a great risk, or simply is not attempted. Beyond the danger of death and long-term disability, infections acquired from surgical procedures degrade confidence in hospital facilities and greatly increase the cost of care. Arguably, standards for surgical patients’ care should not be different anywhere in the world. These standards should be, just like universal precautions, universal – whether they occur in resource-poor or resource-rich settings.
Electricity is a major obstacle to the sterilization of instruments for surgery in LMICs, as the majority of health care settings are not connected to an electric grid. Sterilization technology has seen little progress since it was first introduced, and is still primarily achieved by methods that guzzle electricity and water. Steam-based autoclaves are ubiquitous throughout hospitals and clinics in low-resource countries, but their functionality is limited without unrestricted access to electricity and water. Autoclaves monopolize precious power from generators or solar panels that is needed for lighting and other critical support services throughout a hospital. When they require servicing or repair, as they frequently do, there is rarely anyone in the region with the skills, training or supplies necessary. Furthermore, they degrade plastics and other heat-sensitive materials that are increasingly required for many surgical procedures. For all of these reasons, autoclaves go unused. Instead, health workers must rely on disinfection with chemicals or boiling water.
For example, Pro-Health International (PHI), a faith-based NGO that provides free health care to rural dwellers in Africa (and was co-founded by one of the authors, Dr. Iko Ibanga), endeavors to implement simple and effective infection control measures in its operating unit. PHI would like to ensure that patients, many of whom travel from very far away and may not have another chance to access to a surgeon or doctor, are not getting infected through their instruments. This is very critical for the 70-100 general surgeries and 35-50 ophthalmic surgeries PHI performs during each outreach. (Outreaches are carried out several times in a year.) Presently, PHI sterilizes instruments using an autoclave prior to all free medical outreaches, but as the outreach progresses, disinfection is done using chemicals. Physicians and technicians must work through the constraints of getting adequate and potable water and space to carry out disinfection procedures. But disinfection does not kill all microorganisms, opening up a wide opportunity for infection. Single-use instruments meant to be disposed of after one procedure have been applied as a Band-Aid by international funders, but they are an unsustainable answer.
 The solution to this problem exists in the form of a recently developed portable, power- and water-independent sterilization device, the Eniware Portable Sterilizer, which uses nitrogen dioxide (NO2) gas as a sterilant. The challenge faced by Eniware (which was co-founded by the other author, Dr. James Bernstein) is the rapid distribution and scale-up of the sterilizer to all low-resource health care settings that stand to benefit.
The solution to this problem exists in the form of a recently developed portable, power- and water-independent sterilization device, the Eniware Portable Sterilizer, which uses nitrogen dioxide (NO2) gas as a sterilant. The challenge faced by Eniware (which was co-founded by the other author, Dr. James Bernstein) is the rapid distribution and scale-up of the sterilizer to all low-resource health care settings that stand to benefit.
The ability to sterilize surgical instruments is not only important for surgical care; it acts as a catalyst for improvements in, and expansion of, health care delivery across the entire system. Current reliance on disposable instruments and supplies, and high rates of health care-acquired infection, represent a serious vulnerability for emerging-economy health systems. They hinder everything, from efforts to reduce maternal and child mortality to the scale-up of a simple, proven method of HIV prevention.
The World Health Organization recommended voluntary medical male circumcision (VMMC) as an additional HIV prevention intervention in countries where male circumcision prevalence is low and HIV prevalence is high. Numerous trials and studies have shown the role of VMMC in reducing the risk of female to male transmission of HIV by 60 or more percent. Modeling of the cost and impact of this intervention showed that countries in eastern and southern Africa could avert as many as 3.4 million new HIV infections if the intervention was scaled up to 80 percent of the target age group. Moreover, such scale-up would afford a saving of about $16 billion in treatment cost.
While the global community has progressed in circumcising 6-7 million men, that is far short of the target 20 million PEPFAR set for 2016. Providing the needed circumcision services requires countries to underline the importance of the safety of procedures, cost of supply and environmental protection, among other issues. Most countries use disposal circumcision instrument sets/kits to help in the scale-up. While such pre-packaged instruments address the problem of a lack of sterilization, they create a huge burden on facilities to figure out how and where to dispose of these used instruments, as they take up much-needed space and threaten the safety of the health facility environment for health care workers and community members.
On a recent visit to a remote clinic in Tanzania that is implementing VMMC, it was clear that the costs of using disposable instruments was preventing a simple, inexpensive and extremely effective method of HIV prevention from reaching its potential.
The governments of most countries have a mission and vision to ensure sustainability in their health service programming, a goal to which disposable instrument kits are inherently opposed. Yet these governments have opted to continue with the kits because an age-old challenge – very minimal access to sterilization – prevents most programs from scaling up circumcision using reusable instruments.
Considering the fact that the basic principles behind sterilization were understood in the 19th century, we are long overdue for a technological revolution that will make it available everywhere, starting with portable, power-free sterilization. Safe basic surgery is not a luxury, it is care that virtually every human being will need at some point in their lives, and it is time for us to meet that need in a practical and sustainable way.
Dr. James Bernstein is the co-founder, chairman and CEO of Eniware; Dr. Iko Ibanga is co-founder and director of Pro-Health International.
- Categories
- Health Care
