Healthcare Series: Combining Facilities and Mobile Innovations to Deliver Better Care
Editor’s Note: This post is part of the NextBillion series, Advancing Healthcare With the BoP. Ashoka and The Center for Health Market Innovations are both contributors to the series.
As this series is showing, the challenges of delivering healthcare are being met by extremely innovative ideas, programs and technologies. There is no doubt that there is a plethora of technologies available to address many pressing healthcare delivery issues – from electronic health records, to telemedicine, to novel low-cost diagnostics, to innovations in supply chain and distribution, to the many mobile health devices and applications that are in use around the world today. Training of community health workers, evaluation of health outcomes, data driving both disease surveillance and information for better care – innovation exists in these areas, some including technology and others not. The innovations that leave the greatest impression on me, however, are those that tackle healthcare delivery at the system level. Different technologies and innovations in process working together to address healthcare delivery across multiple aspects of the system is where I believe the real power resides.
Working at Ashoka, with Al Hammond, the co-founder of Healthpoint Services, most of my experience is at the healthcare facility level, especially when it comes to innovations in rural healthcare delivery, a space where Healthpoint and many other players work. Innovations in facility-centered care are many, however, I would still argue that a clinic, a healthpoint, a hospital – are still only one part of the system (granted, a very important part). Over the past year, I have become increasingly familiar with new mobile health tools that are often not a healthcare delivery system in and of itself, but a driver within that system – increasing the knowledge, efficiency, evidence-base, user experience, and accessibility. Still, it is very easy to talk about mhealth over here and facility-based care over there. It is often assumed they both depend on each other, but that dependence is not always addressed directly.
Working with Healthpoint Services, a strategic decision was made not to focus on mhealth tools at the beginning. The focus was to work on the facility-based delivery system including the telemedicine, electric health system (EHR), pharmacy, community health workers, diagnostics and water purification. Now, after 1.5 years of operating, we are making a concerted effort to pilot different mhealth tools, to see which work best, and design the process so that the mhealth systems harmonize with the facility system. Together, they will strengthen each other and increase the opportunities for Healthpoint Services to deliver healthcare.
The healthpoint model has been written about at length here on Nextbillion before (here, here, and here, to name a few), so let’s explore some of the mhealth innovations I am most excited about, keeping in mind that these tools, in my opinion, are optimized when linked with a facility that can incorporate them into their model.
Sensaris SensePack – The idea of combining diagnostics in a small package has been discussed many times before, but this system is different. It combines key medical diagnostic tools – heart rate monitor, glucometer, pulse oximeter, thermometer, and blood pressure monitor – in one small backpack, sensors that sync automatically to a mobile phone, enabling patient test results and other data to be sent across the phone network and added easily to electronic health records.
 The system can send data in batches or one case at a time to a clinic or other healthcare facility – or store the data if cell service is poor. Importantly, the tools are truly simple to use. Healthworkers using the SensPack don’t need sophisticated medical training or even high levels of literacy, and the testing is practically foolproof.
The system can send data in batches or one case at a time to a clinic or other healthcare facility – or store the data if cell service is poor. Importantly, the tools are truly simple to use. Healthworkers using the SensPack don’t need sophisticated medical training or even high levels of literacy, and the testing is practically foolproof.
Community health workers equipped with SensPacks – like those employed by Healthpoint Services – can bring health education to last mile, conducting diagnostic screenings and sharing data seamlessly with Healthpont facilities. Adding mobile health applications and tools to an already existing health infrastructure like the Healthpoint Services clinics creates a reinforcing relationship between two different types of access to healthcare education and services. New sensors and modules – to address the needs of pregnant women and issues of malnutrition as well as others – are also in development.
Fio Corporation’s GenZero – Where point-of-care diagnosis of infectious diseases is needed, or where access to central laboratories is limited, rapid diagnostic tests (RDTs) are quickly becoming the standard of care. RDTs are inexpensive, visually read, and accurate when used by trained healthcare workers in optimal controlled environments. However in practice, sub-optimal conditions can negatively impact RDT accuracy and usefulness. Inadequate training, poor lighting, and fatigue lead to human errors in processing, reading, and capturing data from RDTs. The result is frequent misdiagnosis and poor quality epidemiologic data. Fio Corporation, based in Toronto, Canada, has developed GenZero; a rugged, portable universal reader of existing RDTs. A user places an RDT into GenZero which digitally analyzes the RDT at the optimal time under optimal lighting conditions and delivers an objective diagnostic result – eliminating most sources of human error.  GenZero leverages ubiquitous mobile phone infrastructure and Google’s Android operating system to combine diagnostic results with patient demographic data capable of being transmitted for aggregation. GenZero currently reads malaria RDTs, soon to be followed by HIV, Syphilis, and other infectious disease RDTs. The application of this tool is clear: health workers who want to test for infectious diseases, at the last mile, but who may have limited training or are working in areas where the margin of human error is high, can benefit from these tools. Given the rate of misdiagnosis and overtreatment of certain diseases, these tools will not only increase the ability to provide evidence-based care, but also will help save resources and make sure they are used where needed.
GenZero leverages ubiquitous mobile phone infrastructure and Google’s Android operating system to combine diagnostic results with patient demographic data capable of being transmitted for aggregation. GenZero currently reads malaria RDTs, soon to be followed by HIV, Syphilis, and other infectious disease RDTs. The application of this tool is clear: health workers who want to test for infectious diseases, at the last mile, but who may have limited training or are working in areas where the margin of human error is high, can benefit from these tools. Given the rate of misdiagnosis and overtreatment of certain diseases, these tools will not only increase the ability to provide evidence-based care, but also will help save resources and make sure they are used where needed.
The West Wireless Health Institute’s Sense4Baby platform is another mobile tool that will increase the ability of facilities like those of Healthpoint Services to provide maternal health services efficiently and effectively. 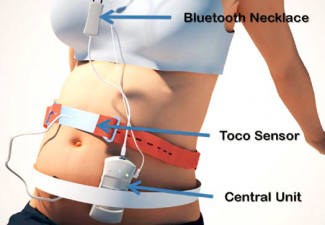 Imagine what happens when a community health worker is alerted to a pregnancy in the community? The health worker provides the Sense4Baby technology to the expectant mother allowing obstetric monitoring to be provided at a distance. Basic training and understanding of the device and its use can create a bridge between the facility and the patient, providing greater opportunities to provide and receive care. The Sense4Baby prototype will be a main component of the “Wireless Pregnancy Remote Monitoring Kit,” which was developed by West Wireless Health Institute, Qualcomm and the Carlos Slim Foundation. The kit is now being tested with community health workers in Mexico.
Imagine what happens when a community health worker is alerted to a pregnancy in the community? The health worker provides the Sense4Baby technology to the expectant mother allowing obstetric monitoring to be provided at a distance. Basic training and understanding of the device and its use can create a bridge between the facility and the patient, providing greater opportunities to provide and receive care. The Sense4Baby prototype will be a main component of the “Wireless Pregnancy Remote Monitoring Kit,” which was developed by West Wireless Health Institute, Qualcomm and the Carlos Slim Foundation. The kit is now being tested with community health workers in Mexico.
- Categories
- Uncategorized
