Why Health Care Remains Poor in NGO-rich Haiti, and How Social Enterprises Can Fix It
Haiti is well known for poor health indicators, underperforming human service institutions and a high concentration of aid-driven actors. Even before the devastating earthquake of 2010, the aid industry in Haiti was crowded with uncoordinated efforts, ranging from multilateral agencies and global NGOs to small-scale organizations and faith-based projects; there are more than 10,000 organizations for a population of just 10 million. No other country in the world has more NGOs per capita. Haiti’s government institutions are chronically under-resourced and, in that void, a robust industry of subsidies and aid has flourished over decades. It has been encouraging in recent years to see a new wave of market-based solutions and social enterprises take root, nurtured by organizations like Yunus Social Business, to demonstrate that an aid culture of free and subsidized goods and services may not be the most favorable strategy for building long-term economic growth and vitality in Haiti.
In the health sector, the marketplace is crowded with a complex web of providers: underperforming public facilities and a bifurcated private sector comprised of NGOs on one end of the spectrum and expensive private practices on the other. Itinerant providers further complicate the marketplace by offering “clinics” for a handful of days by foreign teams throughout the year. Some charity models provide pockets of excellence, like the exceptional service delivery model of Partners in Health in the central plateau. But if you aren’t fortunate enough to live within that geographical catchment area, your options for reliable, high-quality care are limited.
A recent study of primary care coverage and quality across Haiti in the Bulletin of the World Health Organization found that, while 91 percent of the population lived within 5 kilometers of a primary care facility, only 23 percent lived within 5 kilometers of a facility with high-quality service delivery. This study applied a novel, comprehensive approach to the definition of quality, exploring four different quality “domains” comprising 28 indicators.
In Haiti, patients are overwhelmed by a complex set of bad options in a chaotic marketplace which adversely impacts the health-seeking behaviors of vulnerable people. With so little household income to begin with, patients play a game of strategy and risk, often delaying treatment or neglecting care-seeking in the hopes that a visiting clinic or a subsidized option might open nearby.
Remarkably, even with so many service providers, there is a gaping hole in Haiti’s health services landscape for low-cost, high-quality care – delivered in a way that ensures patients are not vulnerable to services cuts once a grant cycle ends. C2C’s community clinic model seeks to fill the gap by providing effective, affordable and quality-assured primary health care services to poor and low-income families in Haiti through a “one-stop-shop” facility: Patients have access to a consultation with a physician, point-of-care diagnostics and an on-site pharmacy. We strive to offer the lowest possible prices to patients and to exponentially improve the value they receive as consumers.
Achieving unit-level sustainability for a health facility that serves a low-income client base is a function of, quite simply, volume and price. But the factors that influence volume and price are anything but simple. Pricing decisions in a Base of the Pyramid market are inherently complex and, in Haiti, they are made more complex by a lack of rational, systematic pricing norms and strategies across the sector. Patient volume is highly variable – not just seasonally, but day to day – which can cause staffing inefficiencies. Health-seeking behaviors are informed by a confluence of price, perception, habit, risk-aversion and lack of knowledge.
Social enterprise models for primary care are gaining tremendous traction in East Africa, India and other emerging markets. Why not Haiti? Funders and innovators alike tend to steer clear of Haiti. “Haiti fatigue” and frustration with the aid industry is widespread. But why not Haiti? A common refrain is that people are simply too poor. And yet, even the public sector in Haiti charges a matrix of user fees. The expectation of payment is there, but the expectation of value is not. We believe that Haitian consumers need and deserve a health service option that fills the current void and delivers value: high-quality, low-cost and not imperiled by donor dependency.
Operating a successful network of clinics in Haiti’s complex market is challenging, but here is what we have learned:
DEMAND CREATION IS PART OF THE CORE BUSINESS
A recent article in the Stanford Social Innovation Review explored the “need-equals-demand” fallacy in social benefit programs. All too often, we assume that goods or services that seem objectively necessary (from our perspective) are needed and wanted by our target customer segment. This approach fails to consider what local information and perceptions drive consumer behavior.
In a market where health knowledge is low and myths abound, educating our target customers about healthy behaviors is part of the core business. Each C2C clinic employs a cadre of community health educators to promote health messaging across the community, through door-to-door marketing and free weekly health screening events. This approach strengthens our links to the communities we serve and keeps the feedback loop strong and current.
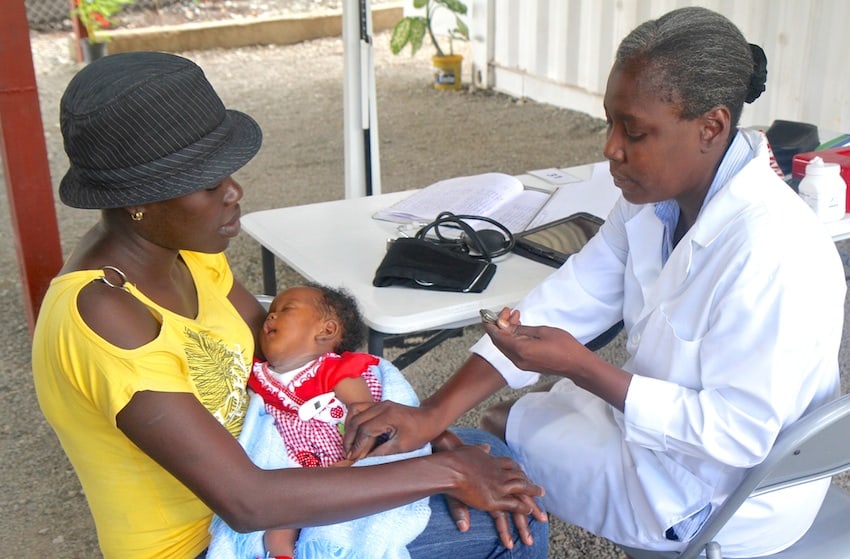
A maternal clinic. All photos courtesy of C2C
BUILD THE BRAND YOUR TARGET CUSTOMER WANTS
Over and over, our patients report that the factor that compels them to choose C2C is “bon accueil” – or, a warm greeting. Years ago, in the program design phase, we assumed that high-quality medical services would drive demand. Through experience and dialogue with our patients, we learned that feeling respected and welcomed when they walk in the door is of the utmost value to them. It sets the tone for the entire patient-clinician interaction and makes patients feel good and more receptive to health information as a result.
At C2C, we integrated the core value of “bon accueil” into our visual brand by adopting a tagline: Sante’w se Priyorite’n (Your Health is Our Priority). But the strategy is more than a tagline. To be effective and authentic, it has to be part of the DNA of the social business, infusing every client interaction.

PRICING IS MORE OF AN ART THAN A SCIENCE
The concept of pricing norms in Haiti is nonexistent. Providers in the marketplace assign prices to health goods and services unsystematically, rarely tied to cost basis and often pegged to an arbitrary interpretation of “what people can afford.” Economists have well established that price functions as a powerful signal to consumers. We hear often from patients about what X or Y service is “supposed to cost,” but in the case of Haiti, these consumer signals – and the associated price sensitivity and preferences – are influenced by an irrational system. This makes operating a health clinic model according to normative business practices an idiosyncratic endeavor. We have found that self-reporting on price expectations or recollection of prices paid in the past is deeply flawed. Some expectations about price are rigid; others are fluid. C2C’s pricing strategy is iterative and highly variable between pharmaceutical and lab products.

PATIENCE
Perfecting a clinic-operating model for a low-income customer segment is a long-term endeavor that requires willingness to experiment, an organizational culture of learning, and patience.
Low-income patients are inherently price sensitive, but they are also fundamentally risk averse, often unwilling to gamble on new experiences because the true cost of spending money at a clinic and not getting well is unbearably high and threatens the whole family structure.
At C2C, we believe that a social enterprise approach to health services in Haiti can work, in time, and that the challenges inherent in the market are surmountable. The work is urgent, because most of the illnesses that threaten the health and wellness of Haitian people are entirely preventable and treatable at the primary care level.
Allison Howard-Berry is the co-founder and executive director of Care 2 Communities (C2C).
- Categories
- Health Care



