Humans Trump Gadgets: How our focus on quick technology wins in global health is distracting us from the fundamental business of health care delivery
In response to the provocative blog post by James Militzer (“Needed: Boring Health Care Solutions”) last month on NextBillion, I would like to add the perspective of a nonprofit organization working in the global health care delivery space today.
The funding community’s thirst for technological solutions in the global health care space has resulted in a manic search for the latest gadget or pharmaceutical reformulation that will serve as a silver bullet in reducing the unnecessary deaths that occur in poor communities around the developing world. We see the private sector’s overemphasis on technology to drive profitability now reflected in the new products capturing the attention of grant-makers and impact investors on the hunt for the ultimate scalable solution.
The superlatives are daunting. Many of the most respected funders in the global health care space have adopted the language (and expectations) of venture capitalists during the explosive growth of the late 1990s. More and more we see grant guidelines searching for “disruptive” “innovative,” “groundbreaking” technologies that have the potential for “global impact” and “scale.” As a result of this skewed attention to feverish growth, it is devices, technology platforms (e.g. mHealth) and reformulated medications that capture the imagination of some of the top funders in the social impact and social innovation space. Somehow the business of health care delivery has fallen by the wayside.
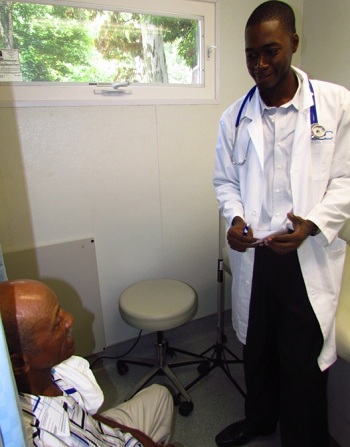
Proper health care is integrated by definition. Think of the hundreds of decisions we make daily to keep ourselves healthy: hand-washing, eating well, drinking enough water, brushing our teeth, not texting while driving, getting enough sleep, taking our allergy meds, the list goes on. Effectively improving the health of a person, a family, a community, requires an integrated health care delivery platform (fancy term) that involves a place for people to receive care when they are sick that also serves up lifesaving information in the form of health education so people can learn to keep themselves and their families healthy.
There is another, less sexy name for this kind of delivery platform: primary care.
According to 2011 World Health Organization statistics:
“Nearly four in every 10 deaths in low-income countries are among children under 15 years. People predominantly die of infectious diseases: Lower respiratory infections, HIV/AIDS, diarrheal diseases, malaria and tuberculosis collectively account for almost one-third of all deaths in these countries.
“Ninety-nine percent of the 6.9 million children who died before reaching their fifth birthday lived in low- and middle-income countries. The major killers of these children were pneumonia, prematurity, birth asphyxia and birth trauma, and diarrheal diseases. Malaria caused about 14 percent of under-5 deaths in sub-Saharan Africa. Maternal deaths have dropped … but are still unacceptably high: Nearly 800 women die due to complications of pregnancy and childbirth every day.”
That’s 2.6 million deaths caused each year by infectious diseases, illnesses that are preventable and treatable. Deaths from these causes can be avoided when people have access to preventative health education about clean drinking water, sanitation, hand-washing and bed nets, as well as to basic health care interventions like condoms, antibiotics, oral rehydration therapy and anti-malarials. And 800 mothers’ lives could be saved each day with access to antenatal care and a trained birth attendant during childbirth in a well-supplied facility.
At Containers 2 Clinics (C2C), we believe the key is delivering these solutions in an integrated, well-functioning, consistent and reliable format – say, for instance, at a primary care clinic that actually opens each day, whose staff is well trained and empowered to do their jobs with functioning medical equipment and a reliable supply chain to keep the clinic stocked with the materials and medications they need. It is these processes and the people who implement and operationalize them daily, working in concert, that are the real lifesavers in these settings.
And, while user fees are a contentious issue in the global health arena, we believe that cost recovery is a critical element of any truly sustainable development solution. Over time, fees will reduce the burden of annual fundraising to maintain clinical operations in perpetuity.
The problem is that primary care is, as Militzer points out in jest, “boring” to funders looking for the cure-all to the top killers in the developing world. Proper primary care is messy, complex, difficult to measure, culturally specific (and therefore difficult to standardize and scale) and, above all, requires patience. But it is the integration of systems – trained personnel, supply, inventory control, maintenance, health education and outreach, demand creation and data collection and synthesis, financial management – that comprise a successful primary care solution in a community and allow it to remain serving that community for years to come.
While health care delivery may be more difficult to track and measure than an innovative device, it is, in fact, the vehicle through which such innovations must pass to reach their beneficiaries. Without a consistent delivery platform, with all its functioning components, even the best technologies will not realize the scale and impact funders seek.
As Ban Ki-moon, U.N. secretary general, once said, “We know what works. … The answers lie in working together to strengthen health systems and ensure universal access to essential services and lifesaving interventions.”
Primary care, despite its pedestrian, common, basic nature, has many of the answers and innovations we need to save lives. The medications are fairly simple, the equipment easy to provide and maintain and the staff are straightforward to train and supervise. I would suggest that the innovation the global primary health arena needs more than anything else is the interest of the media in care delivery models and the patience of funders to see them successfully implemented and supported over time so that these simple solutions can be accessible to the people whose lives are at risk every day.
Jessica Thompson Somol is the executive director of Containers 2 Clinics, which provides comprehensive care to women and children by turning shipping containers into fully-equipped, fully-stocked clinics.
- Categories
- Environment, Health Care, Technology
- Tags
- public health, scale
