Pushing the Boundaries of Health Care Localization: Feb. 5 TweetChat to explore the increasingly disruptive role of technology in serving low-income populations
Many of us working at the intersection of business, technology and social impact have encountered the traditional argument that cultural and market contexts differ across geographies even in the development space. We’ve also heard that it is important to make products/platforms/solutions that embrace these differences. But does this mean that global solutions cannot be created to tackle local problems?
This question came up repeatedly in pilot projects that we have been testing in the field to scale several noninvasive health care devices that leverage mobile, image processing and big data technologies. We want these devices to be global in nature, work just as well in India as they do in Brazil, Nigeria, Kenya, China and other countries, and also contain a built-in ease of distribution to remote locations. Too much localization pushes up costs and becomes a major bottleneck for scale. So we wondered how we could look at things differently and push the boundaries of localization.
As we developed our thoughts further, we arrived at a number of insights hinting at the merit in rethinking delivery and distribution of solutions for rural and underserved markets in various countries. The caveat being, this thinking is most relevant to solutions that are delivered through software and Internet technologies. We created a framework to help guide our thinking, and decided to share with other development and business sector practitioners to hear from them how this can grow.
To arrive at the framework, we divided the “innovation for emerging markets” space into two dimensions – the problem and the solution. It may be noted that both the problem and solution may be global/local/regional or related to developing economies, etc.
Consider this global-local matrix:
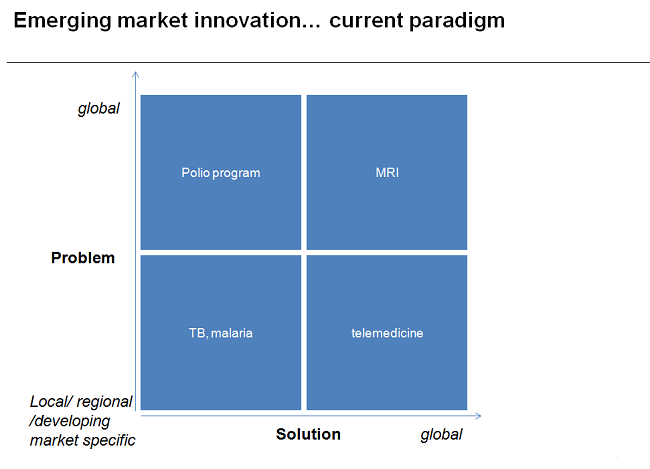
Next, we analysed a few problems. For example, think of MRI machines. The problem they address is global (imaging the brain, etc.) and the way they are built uses a common global technology. Hence, they fit into the upper righthand corner of the matrix. But in developing regions where there is no access to doctors this becomes a very local problem. To address this, lots of global telemedicine solutions like mobile, video conferencing, sensors, etc., have been deployed.
Now look at the top lefthand quadrant. This space pertains to a global problem – say polio – which requires a local solution. Delivery of medicine, for example, becomes a huge issue in poorer nations and a different distribution structure has to be put in place to solve it. The solution in that sense becomes local though the end problem of disease and drug is very much global.
The last quadrant relates to the “local for local” paradigm. Consider tuberculosis (TB) or malaria as examples. These diseases predominantly exist in emerging markets, and hence not many global solutions exist. It is argued that culture and context make this a tough quadrant to tackle. But we think this may not be as big a challenge as it is made out to be.
Allow us to present two approaches that could partially address the “local for local” challenge:
1) Making an engineering trade-off to push more hardware features to the Internet/global platforms:
Let’s continue working with the diagnosis of TB/malaria as an example. Sputum and blood tests are commonly used for diagnosis. The way these tests are carried out may be broken down into two parts: A) how the tests are performed; and B) which technologies are used to perform the tests. It is in part B that we see the role of global platforms.
Micro-fluidic devices, which would be used to analyse blood and sputum, work on a global technology platform with global manufacturing processes. Put another way, a problem involving micro-fluidic devices could find a global solution as shown in red below. This provides the added benefit of opening up more global sales pipelines, and eliminates supporting the associated local R&D costs, which increases the investment justification.
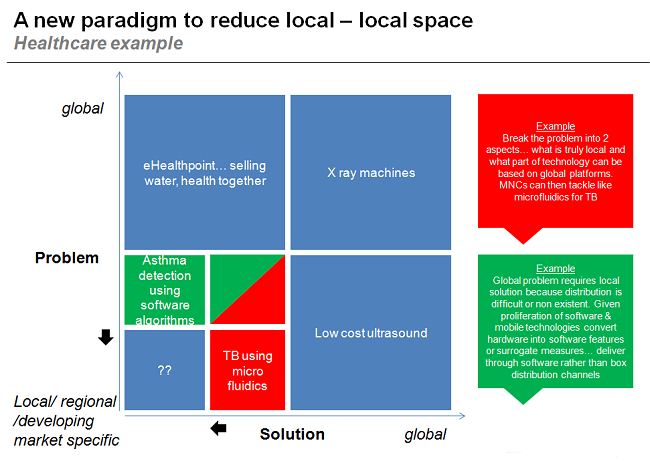
2) Finding Internet-enabled solutions and delivery/distribution mechanisms:
In emerging economies, distribution of solutions is a significant challenge. So can we think of ways in which hardware box solutions may be replaced by software or other solutions that can be taken through existing delivery and distribution channels, i.e. can we modify the solution based on the channel? This is shown as green in the chart above.
Think of mobile technologies that have significantly penetrated emerging markets. Asthma is very prevalent in developing nations, and diagnosing it is a major challenge. If we could use mobile apps to conduct breathing pattern analysis, asthma could, in fact, be detected. See how this eliminates the need for local innovation by globalizing the problem?
The same works in other verticals, too. A case in point is the well-documented story of M-Pesa. The problem M-Pesa sets out to solve is enabling people who don’t have formal bank accounts to conduct safe, everyday transactions. It’s a global problem but locally in Kenya and other emerging markets, banking penetration at the household level is not sufficient and lot of people don’t have bank accounts. Waiting for this penetration/establishment to happen would involve time and significant infrastructure costs. M-Pesa has created an almost parallel infrastructure.
Of course, consumer behavior toward this kind of app needs to be tested, but it is promising in overcoming one aspect of the delivery challenge.
We will be exploring this line of thinking and the increasingly disruptive role that technology will play in health care for low-income and underserved populations in more detail in a live Twitter chat on Wednesday, Feb. 5, starting at 7:30 p.m. India time/5 p.m. Nairobi time/9 a.m. Eastern Standard Time.
Also, catch the full discussion at the open house at the Sankalp Africa Summit in Nairobi, Feb. 12-13, and ongoing conversations at our blog, Aspirational Chasm.
Nisha Dutt is director of consulting services at Intellecap and Harsha Angeri leads and is general manager of business development at Bosch India.
- Categories
- Health Care, Technology
