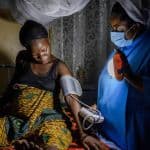
Delivering Family Planning to Rural Customers: Are Mobile Pharmacies ‘Just What the Doctor Ordered’?
Pharmacies serve as key points for quick and consistent access to time- and privacy-sensitive health care products in many emerging markets – family planning (FP) being a key example. When present in rural areas, they can save women from having to spend hours traveling to the closest clinic for a contraceptive prescription, in many cases arriving only to find the clinic is stocked out.
In countries like Malawi, a land-locked East African country experiencing high population growth, they’re growing not only in importance, but in number. The number of Malawian pharmacies has ballooned by nearly 100% in the past 10 years, according to Malawi’s Pharmacy, Medicines and Poisons Board (PMPB). In 2009, the country had just 28 retail pharmacies, compared with over 54 private pharmacies registered with the PMPB in 2018. However, this large growth in retail pharmacies has been mainly concentrated in the urban areas and hasn’t had a noticeable impact in the rural areas. Even in urban centers, the growth has not been evenly spread across the country’s geographic regions, with the Northern Region (the most rural and sparsely populated of Malawi’s three regions) having only nine retail pharmacies. Private pharmacies are clustered in urban centers like Lilongwe and Blantyre, where 69% of Malawi’s retail private pharmacies exist. In contrast, 83% of the country’s population continues to reside in rural areas.
In November 2018, we wrote about our research trip to Malawi, during which we interviewed in-country stakeholders about the private sector’s potential to deliver FP products and services. The goal of this work was to develop recommendations on how the private sector could be utilized to increase FP access for rural women. Free FP services and products are meant to be available widely in Malawi, considering the significant support the country receives from donors. Yet access remains a challenge, particularly for rural women. However, despite the low income of many Malawians and the fact that free public sector products dominate the contraceptive market, there is growing interest in, and use of, the private sector for FP.
As we continued our conversations with in-country stakeholders (e.g. wholesalers, government officials and clinicians) on how to develop solutions to expand the private sector for FP, it became clearer that there is still much to be done to increase access through the private sector. While in Malawi, we met and toured Lilongwe with Mercy Chamwalira, a local pharmacy business owner and economist by training. As a businesswoman whose ventures span both urban and rural settings, Chamwalira provides a unique perspective on how the private sector (and more specifically private pharmacies) could be fostered to expand access to FP, as well as other health care products. We sat down with her to hear her insights on the challenges Malawi continues to face, and potential solutions to increase private sector access for FP products.
The Appeal of Private Sector Family Planning
Chamwalira shared some of the reasons why women are increasingly utilizing the private sector for family planning, and paying for FP products in pharmacies like hers. “The long waiting queues in the public sector make it more convenient for busier and working women to seek services from the private sector where they would rather pay … and not wait long hours,” she explained. “Persistent stock-outs and erratic supply of FP products and other medicines are another [deterrent to relying on public clinics].” Significant privacy and stigma concerns also exist for many women when it comes to accessing contraceptives in the public sector. “Due to cultural norms, some women and youth may not want to be seen receiving FP services, and so they find more privacy in the private sector,” Chamwalira continued.
In the most rural areas of Malawi, women often do not have the option of visiting a private pharmacy for their FP needs due to their sparse availability. It’s effectively a pharmacy desert. Businesses face many challenges in these landscapes, Chamwalira said: “The reason for little presence of the private sector in most rural areas is due to factors such as … poor infrastructure in roads, electricity and telecommunications. Investment in [these challenges] could attract the private sector to expand operations there.”
Mobile Pharmacies: One Answer to Rural Family Planning Access?
How can these obstacles be overcome? One idea that captured strong stakeholder support is a mobile pharmacy solution aimed at circumventing the operational challenges in Malawi’s current landscape for static rural pharmacies. We developed the idea for a mobile pharmacy through a consultative process with in-country stakeholders: It would function as a “pharmacy on wheels” that serves multiple rural areas with FP and other in-demand but difficult-to-access health products. The idea is to balance operational costs while serving the highest possible demand.
While we were in Malawi, we tested our idea of a mobile pharmacy business with Chamwalira and other stakeholders, to get their overall views on its feasibility. To show that there is some precedent for rural populations utilizing mobile services, Chamwalira cited the example of NBS Bank, a local commercial bank, “which runs mobile vans for banking services in the rural areas.” In her view, “Exploring a mobile pharmacy service approach from the private sector for FP products could be a good option.”
However, additional study is needed to determine the optimal business model for this sort of approach – for instance, it could be run as a van with a home base at an existing static pharmacy, or it might be a business without linkage to a brick-and-mortar branch. Market demand, country infrastructure (particularly roads), and community characteristics would be important factors for the ultimate design of a mobile pharmacy model.
Chamwalira’s experience reinforces the conclusion that there is existing demand in rural areas for FP and other pharmaceutical products, despite the widespread idea that little to no purchasing power exists in rural communities. “I am operating a retail pharmacy outside the capital city of Lilongwe [in a trading post], and we absolutely supply women from the surrounding rural areas with FP products,” she explained, as these women travel to her pharmacy because it is the closest available. However, as Chamwalira described it, a purely static rural-based pharmacy may not be feasible from a business perspective in Malawi’s current landscape, since infrastructure challenges significantly increase the cost of running a static business in rural areas: “[Adding a mobile service component] could be a good compromise between offering the service by meeting the existing demand and managing the cost of doing business,” she said. This would work to both maximize access across multiple rural areas, while also maximizing revenue to provide a sustainable business model.
Riding with Chamwalira in her pick-up truck along the dusty pre-rainy season roads of Malawi, we were struck by the immense need and opportunity that exists outside the peri-urban area of Lilongwe. Enabling new rural service delivery models such as mobile pharmacies may be just what the doctor ordered.
Authors’ Note: Support provided by Mercy Chamwalira was greatly appreciated not only in the development of this article but throughout the course of our project “A Total Market Approach to Family Planning: Learning from a Private Sector Wholesaler Landscape Analysis for Malawi.”
Andrea Bare is a Senior Advisor with the William Davidson Institute at the University of Michigan (WDI), NextBillion’s parent organization.
Erika Beidelman is a Research Associate for the Healthcare sector at WDI.
Photo courtesy of Department of Foreign Affairs and Trade via Flickr.
- Categories
- Health Care, Telecommunications