Actually, It IS Brain Surgery
Hydrocephalus is a medical condition in which cerebrospinal fluid (CSF) accumulates in the brain due to a genetic defect, tumors or cysts, fetal hemorrhage or stroke, or neonatal infection. The ailment, which leads to swelling of the head, affects about one in every 500 live births in the US.[1] In developing countries, reliable data are not available; however, the rate is almost certainly higher due to inadequate treatment for neonatal meningitis and other neonatal infections.
Left untreated, hydrocephalus puts pressure on the brain that can lead to brain damage and even death. Without intervention, 50 percent of hydrocephalic children will not survive past their second birthday, and those who live longer often face cognitive disability, spasticity, visual impairment, and head deformity. For the past 40 years, the conventional treatment has been to install a shunt that drains the fluid into another part of the body. Although this is a proven and effective engineering solution to treat this condition, shunts frequently fail. Half fail in the first 24 months and nearly all fail at some point within 10 years.[2]
If you live in Boston or Cleveland, or near a decently equipped community hospital or emergency room, access to neurosurgery to treat this condition is not a problem. However, for most of the world’s population of infant hydrocephalus, the standard treatment involving shunts is effectively a death sentence.
Located in the small, remote town of Mbale in the far eastern part of the country, the CURE Children’s Hospital of Uganda might seem an unlikely place to pioneer a neurosurgery solution. The medical team operates in a resource-scarce environment, yet they’ve found a way to serve their population and the infants afflicted with hydrocephalus. In fact, they are so good at it that the treatment method developed there is being exported to the United States.
Dr. Benjamin Warf served as the hospital’s first medical director. Together with his family, he arrived in Mbale in 2000, only to discover a huge group of untreated pediatric hydrocephalus cases. Early on, he recognized the widespread inability to effectively treat hydrocephalic children due to the cost and the necessary continual monitoring of shunts, and the lack of neurosurgical access for most of Uganda’s pediatric population. So Warf started treating hydrocephalus endoscopically. The endoscopic third ventriculostomy (ETV) approach – using an endoscope to create a hole in the bottom of the third ventricle of the brain – has been used for many years as an alternative approach to shunting. However, ETV was only successful for about 40 percent of the younger babies. Combing through old neurosurgical literature, Dr. Warf explored the use of choroid plexus cauterization (CPC), a seldom-used procedure designed to slow down the production of CSF inside the brain. He first combined these two procedures (ETV-CPC) in 2003, something that had never been done before, and increased the treatment success rate for young babies to over 70 percent. Today, the hospital sees more cases of hydrocephalus than any other place in the world. And that’s because, historically, no other place in the country, or in sub-Saharan Africa for that matter, can offer the kind of treatments that are offered at CURE. Through the CURE Hydro program, there are now 10 other sub-Saharan locations where children are treated using the ETV-CPC technique.
For his groundbreaking work and relentless dedication, Dr. Warf was awarded a MacArthur Fellowship in 2012.
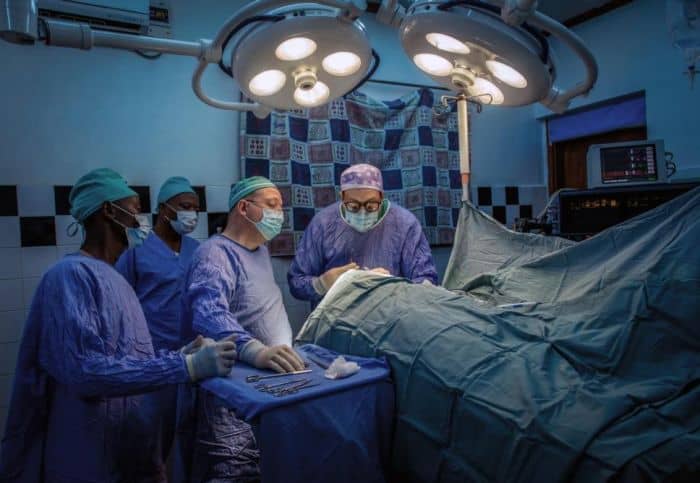
Dr. Benjamin Warf, second from the right, during a surgery at CURE Children’s Hospital in Uganda. (Images courtesy of CURE)
Recognizing the need to scale up this work, Warf simultaneously developed the CURE Hydrocephalus Surgeon Fellowship Program to train neurosurgeons from around the world in the ETV-CPC approach. To date, 24 surgeons from 18 countries have been trained in the ETV-CPC approach to treating hydrocephalus. News has spread throughout the neurosurgical community. Dozens of papers have been published on the results and success. The procedure has gained traction in more industrialized countries, like the U.S. A dozen American pediatric neurosurgeons have traveled to Mbale to learn from the hospital’s team of surgeons how to preform this treatment in order to take it back with them to their hospitals in the states. There are now more than a dozen hospitals and medical academic centers around the U.S. employing the ETV-CPC procedure.
Dr. Warf has since moved back to the U.S. and serves as a neurosurgeon and the Director of Neonatal and Congenital Anomalies Neurosurgery at Boston Children’s Hospital. From there he continues to share his insights gained in Mbale; insights gained from a desperate need in a low-resource setting, but with applications in high-resource settings.
There have been discussions of reverse innovations for many years now and, in a sense, this is but one more example. However, we should never grow tired of learning about them and it is appropriate to celebrate them – especially those that are as life-changing as this. The more people know about the value that is created from innovations in low-resource settings that have applications in high-resource settings, the more we can expect to see.
[1] National Hydrocephalus Foundation, “Facts about Hydrocephalus” http://nhfonline.org/facts-about-hydrocephalus.htm
[2] Warf BC: Pediatric Hydrocephalus in East Africa: Prevalence, Causes, Treatments, and Strategies for the Future. World Neurosurgery:1-4, Summer 2010.
Top image: Dr. Benjamin Warf in front of CURE Children’s Hospital in Uganda.
Paul Clyde is the president of the William Davidson Institute, the Tom Lantos Professor of Business Administration and the Movses and Maija Kaldjian Collegiate Lecturer at the Ross School of Business.
Derek Johnson is the former executive director at CURE Uganda and currently serves as a director for development & sustainability for CURE International.
- Categories
- Health Care, Technology

